Have any questions? Feel free to contact us:
-
Proven
Medical Billing Company Driving Practice SuccessWe offer insights for your practice's billing and revenue cycle, enhancing profitability. As a leading medical billing company, we identify improvement areas to optimize revenue.
-
We specialize in
Providing Comprehensive
Billing Services to small and large practicesOur team is available 24/7 to answer any of your billing questions and concerns
-
Let us
Handle the details of your
Medical Billing So you can focus on patient care.We understand the importance of patient privacy and security. Our team is committed to protecting your data.
-
We are committed to providing
Quality Service and excellent customer support.We understand the importance of accurate and timely payments. Let us help you maximize your reimbursements.
-
Now Introducing!
GreenSense
Financial SolutionsGet on our waiting list :
- Pre-Funding
- Interest-Free Loans
Expert Medical Billing Company Maximizing Reimbursements

About US
GreenSense Billing is a small family company with big ideas to serve our clients. We understand that medical providers often face a burden of paperwork and challenges in getting paid for their services. Our team has over 20 years of collective experience in medical billing and collections, and we use proven techniques and effective denial management to maximize payment for our clients. By offering these services, we aim to help our clients streamline their billing processes and focus on providing quality care to their patients.
Optimized Healthcare Operations with Our Premier Medical Billing Company
Imagine elevating your healthcare practice’s efficiency and patient care quality by partnering with GreenSense, a top-tier medical billing company in usa. This invaluable partnership guarantees smooth patient care processes while ensuring you receive timely payments without a hitch.
Introducing our adept team of U.S.-based medical billing professionals, each member is an expert with extensive experience in handling sophisticated electronic health record (EHR) systems. With their support, witness your practice undergo a transformation into a streamlined and innovative operation. This change allows you to concentrate solely on providing exceptional care to your patients, with the added assurance of secure and prompt payment transactions.
Our proprietary software is meticulously designed to enhance operational efficiency and accuracy. It plays a pivotal role in improving revenue cycle management, safeguarding data, enhancing patient experience, minimizing administrative tasks, providing insightful reporting and analysis, and offering seamless integration with various systems.
GreenSense stands out as a premier healthcare billing company committed to empowering your healthcare practice. We take the reins of the medical billing process, ensuring each bill is paid on time and every financial aspect is meticulously managed. Our intuitive dashboard and patient-centric tools simplify the billing process, allowing for effortless management of appointments, schedules, billing codes, financial reports, and more. With GreenSense, medical billing is no longer a daunting task but a streamlined process, enabling you to deliver the best patient care with ease.

We are Medical Billing Company Offering Full Suite of Features
Practice Management Software
Our medical billing software helps manage appointments, patient registration, claims submission, and payment collection. It is trusted by healthcare professionals and has advanced efficiency, accuracy, and security features.
EHR Software Tool
Our medical billing software streamlines billing tasks with automation and efficiency. It is a user-friendly EHR tool that helps improve healthcare standards and optimize billing processes.
Patient Portal
We provide an integrated patient engagement portal for medical billing and coding experts. It allows real-time access to information and helps you stay connected with your patients.
Managed Billing Services
Managed billing services can help practices save money in the long run by optimizing billing processes and reducing the risk of errors and denied claims. This can translate into higher revenue for the practice and more financial stability.
Easy User Interface Dashboard
Our platform includes smart dashboards that allow you to easily monitor and analyze your billing and revenue progress through simple navigation tools.
Patient Engagement Tool
Stay connected with all your patients and get engaged with them through your patient engagement tool
Financial Data Analytics
You can now access real-time data analytics for all your financial information and see how well are you performing in your revenue generation
Patient Cards
With special electronic patient cards, you can easily offer a more convenient way to be able to manage or share patient data
Reminder Alerts
You can even set reminder alerts to always set ahead before scheduling any appointment, simplifying workload tasks and working out your priorities
Reputation Management
Manage your online reputation of your medical practice with reputation management which helps you submit and collect patient reviews and survey to capitalize on your goodwill and medical success reputation
ePrescribing
You can prescribe medications more safely and effectively while analyzing, review and keeping track of all your patient information, medical history and treatment plans with EHR software tool
Telemedicine
You can satisfy your patients with telemedicine and extensive care coverage with reduce costs
Revenue Cycle Management Services
Reliable Convenience for All Your Billing Hassles
With GreenSense Billing, you can conveniently access your medical data and stay in touch with your patients, no matter where you are. Our platform offers features for handling appointments, treatment plans, reports, and scheduling changes. As a trusted and reliable company, we are committed to helping you establish strong relationships with your patients and providing user-friendly solutions for your health billing needs.
Elaborate and Complete
Our services is designed to provide a comprehensive and user-friendly solution for optimizing your billing processes and improving efficiency. Whether you are dealing with insurance claims, patient billing, or other financial matters, our team of experts is here to help you succeed and provide the best possible care to your patients.
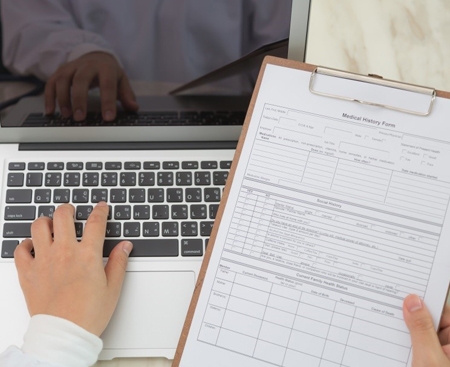

Better Interoperability
We help medical practices with their billing and financial management by providing services such as managing payments and tracking patient information. We also offer data analytics to help practices understand and improve their financial performance.

Real-time Intelligence
All your medical billing and medical claim processing and workflows are automated to provide real-time information which is accurate and 100% error-free
Tips for Leak-Proofing Revenue
Shore up your check-in process
Patient check-in is a critical point to your revenue cycle. That is why you need Revenue Cycle Management Services. You just have to search “Medical Billing Services Near Me” and GreenSense will be there to help you out. If you’re not able to quickly pull up patient information, copays, and balances due at check-in, you’re going to be leaking cash all over the place. Here’s the source of the most common leaks:
- Failing to verify patient information
- Not knowing or having to search for the right co-pay amount
- Not knowing if the patient has a balance due
- Not checking patient insurance benefits
- Failing to get authorizations before providing services
- Not giving patients convenient payment options like online paying or credit card on file
Double check claims
Claims denials are responsible for lots of lost time and money. With the transition to ICD-10, it’s more important than ever to double check claims. Green Sense Billing gives you a perfect Solutions to help you manage your entire claims process in one place. You’ll save money by streamlining and managing your claims better than ever before through our services.
Improve your collections
Collecting the money that you’re owed is the best way to close bad debt holes and capture lost revenue. Modern patient portal tools within Patient, integrated with the expertise of a top-tier medical billing company, give you several money-saving solutions to improve your collections. The portal is seamlessly integrated with our EHR and practice management for one cohesive revenue-collecting solution. All that is required is a link from your practice website, an internet connection, and authorization to access the patient portal.

Latest Blog
How Important is Cybersecurity for Your Clinical Practice?
April 22, 2024
MACRA & MIPS: Best Practices to Improve Your Practice
April 19, 2024
Customer Reviews
I am extremely pleased with GreenSense Billing. My account has been handled by a team of extremely diligent resources who are very quick with communication. They followed up on all billing transactions immediately and I am getting paid reliably by insurance companies. I get answers to all my questions and receive excel sheets to better explain all steps of billing transactions in great detail. GreenSense Billing has handled my credentialing process very smoothly. Things are going so well I have asked them to expand my insurance coverage and look forward to growing my practice. Their professionalism and reliability make them excellent to work with. Highly recommend GreenSense Billing. My practice has flourished in the last 3 months since hiring GreenSense Billing.
Dr. Rajsree
MD.
I cannot sing the praises of GreenSense Billing enough. They are knowledgeable, professional, and responsive. I am super glad to have contacted them to take care of our business. It is an absolute pleasure working with you. The transition to your company was effortless and seamless. Definitely one of the best medical billing companies near me!
Elizabeth Abraham
Office Manager
I have been using GreenSense Billing as my billing company, they are professional, helpful and hardworking people. They respond and answer all my questions on time . They are excellent in billing and collections, I highly recommend them.
Dr. Fady Fayad
Office Manager
We have recently changed our billing to GreenSense Billing and Advanced MD and the experience has been greatly positive.
The implementation phase was smooth and painless. We had the pleasure to work directly with the key players in their team who helped us create and upload all our patient intake forms and all insurance information required. Our transition from previous biller to GreenSense Billing was seamless and effective. We highly recommend GreenSense Billing.
Dr. Tano
MD.
Start generating more revenue from your collections and minimize your overhead costs.